Starting a fertility journey can feel overwhelming, especially when you are unsure where to begin or whom to trust. With so many clinics, treatments, and opinions available online, choosing the right specialist often becomes one of the hardest parts of the process.
Most people searching for the best fertility doctor are not only looking for qualifications or technology. They are looking for someone who listens carefully, explains things honestly, and makes them feel supported during a deeply personal phase of life.
The World Health Organization has also emphasized the importance of evidence-based infertility diagnosis and treatment guidelines to improve access to quality fertility care worldwide.
If you are trying to find the right fertility expert in Vizag, focusing on a few important factors can make the decision much easier and more confident.
Start by Looking at Experience and Specialization
Experience matters in fertility care because every case is different. Some couples may struggle with ovulation issues, while others may face male fertility concerns, hormonal imbalances, or unexplained infertility.
A doctor who has handled a wide range of fertility cases is often better equipped to recommend the right treatment approach without unnecessary delays. While searching for the best fertility doctor, take time to look into the doctor’s background, years of practice, and areas of specialization.
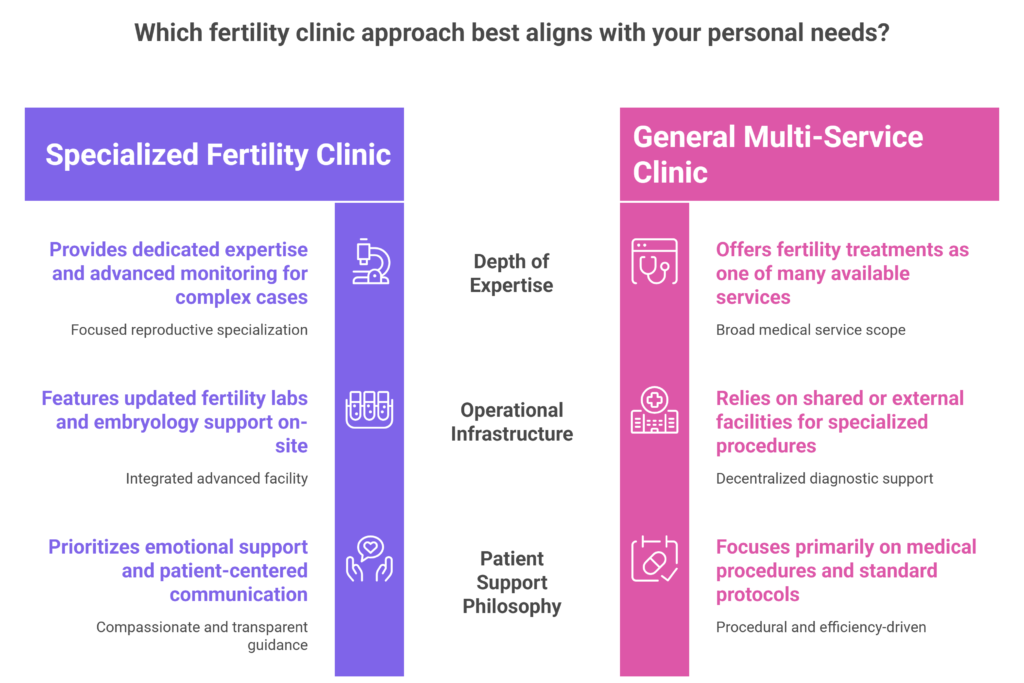
It also helps to check whether the clinic focuses specifically on fertility treatments rather than offering them as just one of many services. Fertility care requires dedicated expertise, advanced monitoring, and continuous support throughout the process.
The Best Fertility Doctor Will Prioritize Patient Care
The best fertility treatment experience is not only about medical procedures. Communication and emotional support also play a huge role. During consultations, notice how the doctor interacts with you.
A good fertility doctor understands that patients often arrive with anxiety, confusion, and emotional stress. Instead of pushing treatments immediately, they take time to understand medical history, lifestyle factors, and personal concerns before suggesting a plan.
Read Reviews Carefully but Realistically
Online reviews can offer useful insight, but they should not be your only deciding factor. Instead of focusing only on star ratings, read the detailed comments. Patients often mention whether the doctor was approachable, transparent about costs, supportive during treatment, and available for follow-up questions. These details matter more than generic praise.
At the same time, it is important to stay realistic. Fertility treatments do not guarantee instant success, and even the most experienced doctors cannot promise outcomes. A few negative reviews do not automatically indicate poor care. Look for overall consistency in patient experiences rather than isolated comments.
Look for Transparent Treatment Guidance
One of the biggest concerns for couples is uncertainty around treatment plans and costs. A trustworthy clinic will explain why a particular test or treatment is being recommended. They will discuss timelines honestly and help you understand possible outcomes without creating unrealistic expectations.
Whether it involves medication, IUI, or In Vitro Fertilization, transparency matters at every stage. Understanding the financial side of treatment is equally important, which is why many couples spend time researching topics like IVF pricing and treatment inclusions before making a decision. Resources such as Understanding IVF Costs in Vizag: A Comprehensive Guide can help patients get a clearer picture of what to expect.
The best fertility doctor will focus on what is medically appropriate for your situation rather than suggesting aggressive treatments immediately.
Consider the Technology and Facilities Available
Modern fertility care depends heavily on accurate diagnosis and advanced lab support. When evaluating clinics in Vizag, check whether they have updated fertility labs, ultrasound facilities, and embryology support available within the center itself. Clinics with advanced infrastructure can often provide smoother coordination and better monitoring during treatment cycles.
That said, technology alone should not be the deciding factor. Even the most advanced equipment works best when combined with skilled medical judgment and personalized care.
Pay Attention to Accessibility and Follow-Up Care
Fertility treatment usually involves multiple visits, scans, and follow-up appointments. Choosing a clinic that is accessible and responsive can make the process far less stressful. Many patients overlook this aspect initially and later struggle with long waiting times or difficulty reaching the doctor during important stages of treatment.
The best fertility doctor is someone whose team communicates clearly, schedules appointments efficiently, and provides guidance when patients need reassurance or clarification.

Finding the best fertility doctor in Vizag is not about choosing the clinic with the biggest advertisements or the most promises. It is about finding a specialist who combines medical expertise with honesty, patience, and compassionate care.
Fertility journeys can take time, and having the right doctor beside you can make that journey feel far more manageable. Take time to research, ask questions, and understand your options before making a decision.
If you are searching for the best fertility doctor in Vizag, choosing a clinic that combines experience, transparency, and compassionate care can make all the difference. Book an appointment with London IVF Centre and take the first step toward expert fertility guidance and personalized care.
May 12, 2026
Most people think that pregnancy will happen naturally when the time is right. And for many people, this is the way it happens. But for others, the journey takes longer, feels uncertain, and often comes with more questions than answers.
In fact, according to the National Health Service (NHS) UK, around 1 in 7 couples may have difficulty conceiving. Which means if you are feeling unsure or concerned, you are not alone in this.
If you are trying to get pregnant and not succeeding, then you might have a doubt- should we keep trying or consult a fertility doctor?
The truth is, knowing when to seek help can make a meaningful difference. A timely consultation with a fertility doctor is not about rushing the process. It is about understanding your body better and making informed decisions early on.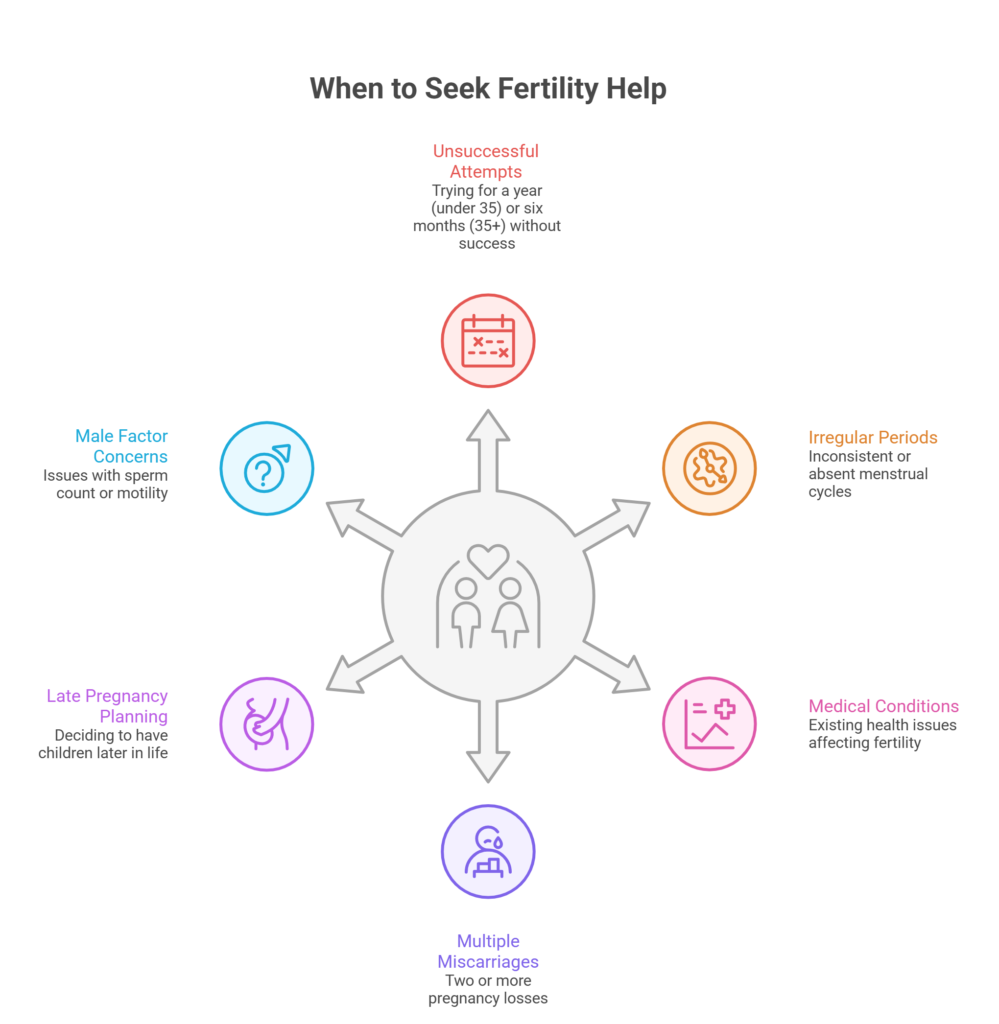
You Have Been Trying Without Success
The first and most obvious sign is that you have been trying for quite some time and are not getting a positive result. If you are under 35 and it has been a year of trying without a result, it is usually a good point to check in with a doctor. If you are 35 or older, that timeline tends to shorten to around six months.
This happens because fertility naturally declines with age, especially when it comes to egg quality and quantity. What may simply take a little longer in your late twenties can start to need support as you move into your mid to late thirties. Reaching this point does not necessarily mean something is wrong. It simply means it may be time to understand what could be happening more clearly.
Your Periods Are Irregular or Absent
Your menstrual cycle is often one of the most important indicators of your reproductive health. If your periods are highly irregular, very far apart, unusually heavy, or even absent, it could point to issues with ovulation. And without regular ovulation, getting pregnant can become more difficult.
Conditions like Polycystic Ovary Syndrome are a common reason behind irregular cycles, and hormonal imbalances also play a role in irregular periods. Many people ignore these signs for years, assuming it is just how their body functions. But if you are planning to get pregnant, you need to consult a fertility doctor and get these patterns checked at the earliest.
You Have Known Medical Conditions
Certain health conditions can directly or indirectly affect fertility. For example, Endometriosis can impact the reproductive organs and make conception more challenging. Thyroid disorders, diabetes, and other hormonal issues can also interfere with ovulation and implantation.
Even past pelvic infections or surgeries can sometimes lead to complications. If you already know you have any of these conditions, it is better not to take a wait-and-watch approach. Early guidance from a fertility doctor can help you understand your options and avoid unnecessary delays.
You Have Experienced Multiple Miscarriages
While a single miscarriage can be fairly common, having two or more may point to an underlying issue that needs attention. This could be linked to genetics, hormone levels, or structural concerns within the uterus.
Seeking help at this stage is about getting clarity and the right support, not overreacting. In many cases, understanding the cause can make a meaningful difference to your chances of a healthy pregnancy going forward.
You Are Planning Pregnancy Later in Life
More people today are choosing to start their families later, and that is completely understandable. At the same time, it does come with certain biological factors.
Fertility does decline with age, especially after 35. This does not mean pregnancy is not possible, but it may take longer or need a bit of medical support. Read more about getting pregnant after 35 here.
Speaking to a fertility doctor early can help you understand where you stand and what options you have. Treatments like In Vitro Fertilization(IVF) are often part of that conversation, not as a last resort, but as one of several possible paths.
Male Factor Concerns
Fertility is often seen as a woman’s health issue, but that is only part of the story, as male factors contribute to a significant share of infertility cases. Issues like low sperm count, poor motility, or past medical conditions can all play a role. Lifestyle habits such as smoking, alcohol use, and ongoing stress can also affect sperm health.
If there are any concerns on the male side, it helps to look into them early. Fertility involves both partners, and both need to be equally involved in the process.
When Not to Panic Yet
It is equally important to understand that not every delay points to a problem, especially if you have only recently started trying. It is completely normal for conception to take a few months, and factors like stress, timing, and even chance can all influence the process.
What really matters is finding a sense of balance, where you do not jump to conclusions based on random information online. At the same time, do not overlook consistent signs that may need attention.
Deciding to see a fertility doctor can feel like a big step. But it is not a sign of failure or something being “wrong.” In many cases, it is simply about getting the right guidance at the right time. The earlier you understand your body and your options, the more confident and informed your decisions can be.
If you have been waiting, wondering, or quietly worrying, it might be time to get some clarity. Reach out to London IVF Centre and take the next step with the right guidance and care.
April 28, 2026
If you have been trying to get pregnant for some time without any success, then there is a high probability that you might have undergone some fertility tests. Your fertility test will have a lot of numbers and a lot of medical terms that can make you anxious. A fertility test might leave you with more questions than answers. Is this normal? Is that number too low? Does this mean something is wrong with my partner or me?
Without the right explanation, fertility tests can create a lot of confusion and panic, especially when you are already stressed about trying to get pregnant. Let’s understand more about the fertility tests, why they are prescribed, which are the common fertility tests, how to read them, and mistakes to avoid while interpreting the results.
Why are Fertility Tests Done?
Your fertility doctor will get a fertility test done to build a clearer picture of what is happening in your body. For women, that picture includes how many eggs are in reserve, whether ovulation is happening as expected, how hormones are behaving, and whether the uterus and fallopian tubes look healthy. For men, it focuses on the quality and quantity of sperm. This kind of evaluation is very common because, according to the World Health Organization, about one in six people worldwide experience infertility at some point in their lives.
Common Tests for Women and What They Mean
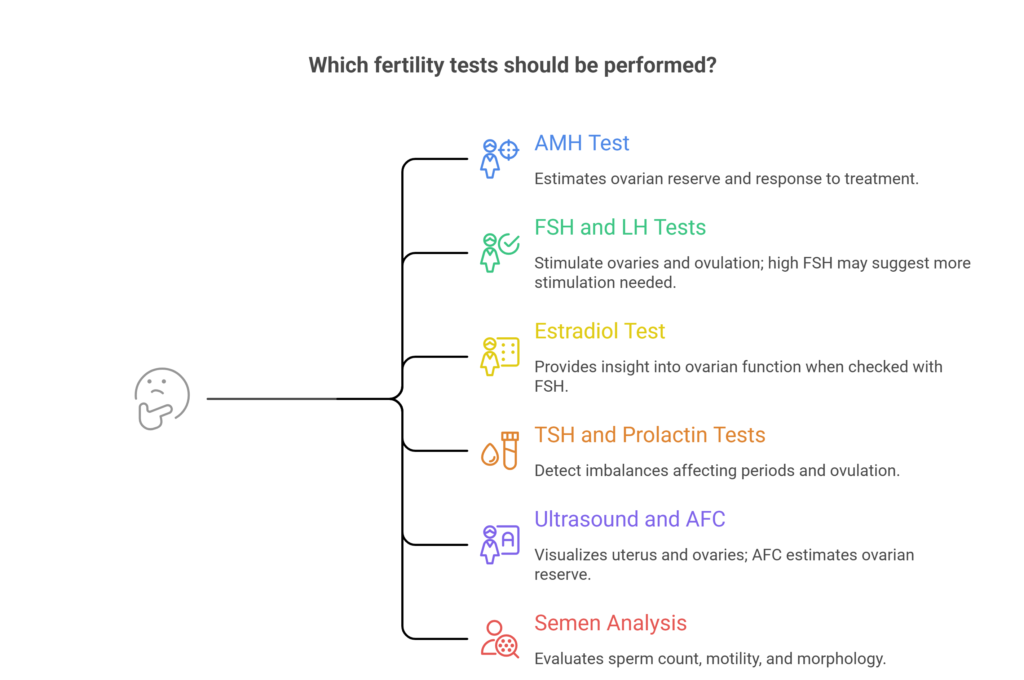
Most women start with a set of blood tests and an ultrasound. Here are some of the common fertility tests.
Anti-Müllerian Hormone (AMH)
AMH gives an idea about ovarian reserve, which means how many eggs are left. A low AMH does not mean you cannot get pregnant, and a high AMH does not guarantee easy conception. It only helps doctors estimate how your ovaries might respond to treatment and how to plan the next steps.
Follicle Stimulating Hormone (FSH) and Luteinizing Hormone (LH)
These hormones are usually checked on day two or three of your cycle. FSH helps stimulate the ovaries, and LH plays a role in ovulation. If FSH is higher than expected, it can suggest that the ovaries need more stimulation to work. This does not mean pregnancy is impossible; it simply helps guide treatment decisions.
Estradiol (E2)
Estradiol is a form of estrogen that is often checked along with FSH because the two values together give better insight into how the ovaries are functioning in that cycle.
Thyroid Stimulating Hormone (TSH) and Prolactin
Thyroid and prolactin levels can quietly affect periods and ovulation. Even small imbalances can interfere with regular cycles, which is why these tests are part of a basic fertility workup.
Ultrasound and Antral Follicle Count (AFC)
An ultrasound helps doctors look at the uterus and ovaries. The antral follicle count is a simple count of small follicles seen in the ovaries at the start of a cycle. Like AMH, this gives an idea about ovarian reserve, but it can vary from month to month.
Common Fertility Tests for Men and How to Read Them
For men, the main fertility test is a semen analysis. This report usually talks about three key things.
-
Count means how many sperm are present.
-
Motility means how well they move.
-
Morphology means how many have a normal shape.
Semen quality can fluctuate significantly based on recent illness, stress, a high fever in the weeks before the test, or even dehydration. Since sperm count is one of the most common concerns that shows up in a fertility test, you can also read our detailed guide on Low Sperm Count: Signs, Causes, and Treatment Options to understand what it means and what can be done about it.
What “Normal” and “Abnormal” Really Mean
One of the most stressful parts of reading a fertility test report is seeing values marked outside the reference range. They are statistical averages based on large populations, and being slightly outside the range does not mean that everything is wrong. Your fertility doctor will look at patterns, symptoms, medical history, age, and how long you have been trying to conceive.
What Your Results Can and Cannot Tell You
Fertility tests can help identify issues like ovulation problems, hormone imbalances, low ovarian reserve, or sperm-related concerns. They also help your doctor decide what kind of treatment makes sense and when to move forward.
What they cannot do is predict the exact moment you will conceive or guarantee any outcome. They also cannot measure things like emotional readiness, stress levels, or the many small factors that affect real-life fertility.
Common Mistakes People Make When Reading Reports
One of the biggest mistakes is comparing your numbers with someone else’s. Every person’s body is different, and every fertility journey is different. Another common mistake is assuming that a low or borderline value means there is no hope. In reality, many people conceive with numbers that are not perfect, sometimes with help and sometimes naturally.
How to Talk to Your Doctor
You can ask what each result means for you, what your options are, and whether you need repeat tests or further evaluation. It is completely okay to ask for an explanation in simple language. A good consultation should leave you feeling clearer, not more confused.
Fertility test results can feel overwhelming, but they are the beginning of a more informed and more personalised fertility plan. At London IVF, we take the time to sit with you, walk through your results properly, and help you understand what they mean for your specific journey. If you would like to review your results with us, book a consultation and let us help you take the next step with clarity.
March 1, 2026
If you are trying to get pregnant and everything seems to be in place, the journey can still feel unexpectedly difficult. When your medical tests come back normal, and pregnancy still does not happen, the lack of a clear explanation can feel overwhelming. When there is no clear medical explanation, you might be told you have unexplained infertility, a term that can feel confusing and frustrating at the same time.
Unexplained infertility is more common than many people realise; in fact, research shows that about 30 percent of couples struggling to conceive are diagnosed with unexplained infertility.
What Does Unexplained Infertility Mean?
Unexplained infertility is diagnosed when standard fertility evaluations do not reveal an obvious reason for not being able to conceive. This usually means that ovulation appears regular, the fallopian tubes are open, the uterus looks normal, and semen analysis results fall within expected ranges.
It is important to understand that this diagnosis does not mean “nothing is wrong.” It simply means that current testing methods have not identified a clear issue. Fertility is complex, and not every factor can be measured with routine tests.
Why Pregnancy May Not Happen Even When Tests Are Normal
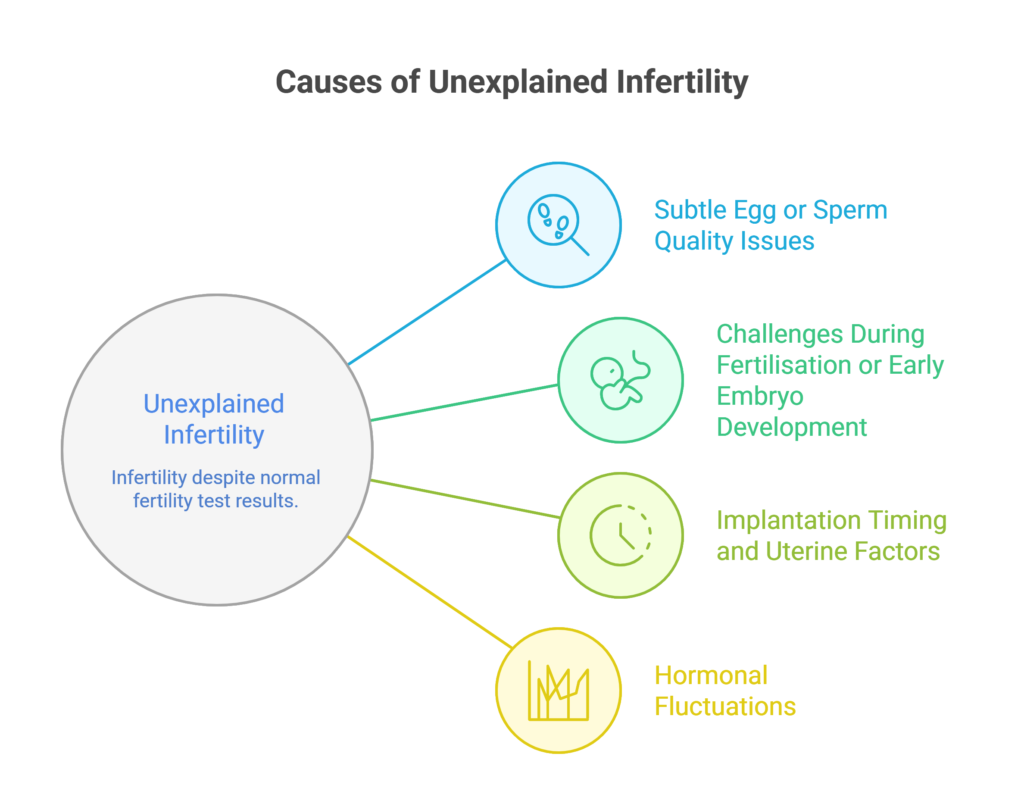
Just because the routine fertility tests turn out to be normal does not mean that everything is fine. There are other factors to consider as well, including:
Subtle Egg or Sperm Quality Issues
Standard fertility tests assess quantity and basic function, but they cannot always detect subtle quality concerns. Eggs and sperm may appear normal on routine testing, yet still have microscopic or genetic issues that affect fertilisation or embryo development.
Challenges During Fertilisation or Early Embryo Development
Even when ovulation and sperm parameters are normal, fertilisation may not always occur as expected. In some cases, fertilisation happens, but embryo development slows or stops before implantation. These early-stage challenges are difficult to detect because they occur before pregnancy can be confirmed.
Implantation Timing and Uterine Factors
For pregnancy to occur, a healthy embryo must implant into the uterine lining at precisely the right time. Small variations in uterine receptivity, blood flow, or lining development can affect this process.
Hormonal Fluctuations
Hormone levels naturally fluctuate from cycle to cycle. Even when hormone tests fall within normal ranges, small timing differences can affect ovulation quality or implantation. These subtle variations can contribute to unexplained infertility.
The Role of Age in Unexplained Infertility
As your age increases, unexplained infertility becomes more common. While tests may still appear normal, egg quality naturally declines over time. This can lead to fertilisation or implantation challenges that are not easily detected through routine evaluations.
This does not mean that you cannot get pregnant, it simply changes how fertility is assessed and how treatment plans are designed. Early evaluation and timely decision-making are important in such cases.
The Emotional Impact of an Unexplained Diagnosis
After months of trying and undergoing multiple medical tests, an unexplained diagnosis can be emotionally exhausting. You might feel confused, helpless, or even guilty, wondering if you have missed something or waited too long.
Fertility challenges affect not only the body but also mental and emotional well-being. Support from medical professionals, counsellors, and trusted loved ones can help you navigate this uncertainty with greater confidence.
What Are the Next Steps After a Diagnosis?
After diagnosing unexplained infertility, doctors usually review the complete fertility history rather than focusing on a single test result. This includes factors such as age, how long you have been trying, menstrual patterns, and any previous pregnancies or treatments. Treatment options vary based on individual situations. Some couples benefit from closer cycle monitoring to optimise timing, while others might need more advanced support.
If you want a clearer picture of how fertility care is planned, this step-by-step IVF treatment guide from consultation to conception can help explain what the process typically looks like.
Why Personalised Care Is Important in Unexplained Infertility
There is no single approach that works for every case of unexplained infertility. What works for one couple may not be suitable for another. Your age, how long you’ve been trying, your medical history, and how you respond to initial interventions all shape the next steps.
This is where specialist fertility clinics like London IVF Centre make a real difference. They can identify subtle patterns that general practitioners might miss and adjust treatment approaches based on how your body responds.
When to Seek Further Guidance
If pregnancy has not occurred after a reasonable period of trying, or if uncertainty is causing significant stress, seeking guidance from a fertility specialist can be helpful. Even when previous tests appear normal, a fresh evaluation or second opinion may provide new insight.
Time does play a role in fertility, so delaying decisions for too long may not always be helpful. At the same time, it is just as important not to rush into treatments you do not fully understand or feel ready for.
Many couples diagnosed with unexplained fertility go on to conceive with the right guidance and support. With a thoughtful, personalised approach and clear communication, you can take the next steps without feeling rushed or overwhelmed.
Understanding unexplained infertility can feel overwhelming. At London IVF Centre, our specialists take time to listen, explain your options, and support you with a personalised care plan based on your needs. Book a consultation to discuss your options in detail.
February 17, 2026
If you have started discussing fertility treatments, then age must have been one of the first few things your fertility specialist must have talked to you about. Like many couples, you also must have felt that if you are healthy, age will not play a major role in your ability to conceive. While good health does matter, age has a direct impact on fertility in ways that are not always visible. Understanding how age influences fertility treatment can help you make informed, timely decisions without unnecessary fear or pressure.
How Age Affects Female Fertility and Fertility Treatment
Women are born with a fixed number of eggs, and both the quantity and quality of these eggs naturally decline over time. In the early 20s, fertility is generally at its peak. From the early 30s, egg numbers begin to reduce gradually, and after 35, this decline becomes more noticeable. By the early 40s, both egg quality and availability can drop significantly. Research shows that female fertility starts to decline around the age of 32 and drops more sharply after the age of 37, largely due to changes in egg quality and quantity.
This does not mean pregnancy stops after a certain age, and many women conceive later in life. As egg quality declines, the chances of fertilisation, implantation, and a healthy pregnancy can be reduced. The risk of miscarriage also increases with age. These are natural biological changes and not a reflection of overall health or lifestyle.
How Age Affects Male Fertility
Fertility discussions often focus on women, but male age matters too. Although men continue to produce sperm throughout life, sperm quality can change with time. Factors such as reduced motility and higher DNA fragmentation become more common with age, especially after forty. Read more about the signs, causes, and treatment options for low sperm count here.
These changes may not always show up clearly in routine semen tests, but they can influence embryo development. That is why fertility specialists increasingly consider both partners’ ages rather than viewing fertility as a woman’s only issue.
How Age Affects Fertility Test Results
Fertility tests help doctors understand how the reproductive system is functioning at a given point in time. Tests like Anti-Müllerian Hormone (AMH) levels, ultrasound follicle counts, and hormone panels are all influenced by age.
A low AMH does not mean pregnancy is impossible, just as a normal result does not guarantee success. These tests help doctors choose the most suitable treatment approach and timeline, especially when age is a factor.
Why Age Influences Treatment Success
One reason age affects fertility treatment outcomes is embryo quality. Younger eggs are more likely to develop into embryos that implant successfully and continue into a healthy pregnancy. As age increases, the likelihood of embryos with chromosomal abnormalities also rises.
Delaying evaluation or treatment when fertility markers are already declining may limit certain options later. Early assessment gives doctors more flexibility in choosing the most suitable approach.
Fertility Treatment Options at Different Ages
There is no single treatment that fits everyone of a certain age. Younger women may respond well to simpler treatments, while women in their late 30s or early 40s may benefit from more advanced approaches. What matters is how age interacts with ovarian reserve, overall health, and previous treatment response.
A personalised approach ensures that treatment decisions are based on individual needs rather than assumptions. Two women of the same age may require very different treatment plans.
The Emotional Side of Age-Related Fertility Concerns
Age-related fertility discussions can be emotionally challenging. Many people experience guilt, anxiety, or regret, especially if they delayed trying to conceive for personal or professional reasons. These feelings are common and understandable.
It is important to remember that fertility journeys are deeply personal. Emotional support, clear communication with doctors, and realistic expectations can help reduce stress and make the process more manageable.
Why Early Evaluation Makes a Difference
Early fertility evaluation does not mean starting treatment immediately. Taking an early evaluation can help you plan, explore options, and make decisions without urgency or panic.
Age matters in fertility treatment because it shapes how the body responds, how treatments are planned, and how outcomes are interpreted. With the right guidance, many people achieve healthy pregnancies at different stages of life.
If you have questions about how age may affect your fertility, the specialists at London IVF Centre are here to guide you. A personalised consultation can help you understand your options and plan your next steps with confidence.
January 18, 2026
Like many couples starting their fertility journey, you and your partner must have undergone Intrauterine Insemination (IUI). IUI is less invasive than In Vitro Fertilization (IVF), more affordable, and seems like a natural first step for most couples. If you have already gone through one or more IUI cycles without success, you might be wondering whether to try IUI again or move on to IVF.
Knowing when to shift from IUI to IVF helps save precious time, reduce emotional strain, and sometimes even lower overall costs. This blog is designed to help couples make a clear and informed decision, especially those seeking fertility treatment in cities like Visakhapatnam, Kakinada, Rajahmundry, Vizianagaram, and Ankapalli.
Understanding the Difference Between IUI and IVF
IUI involves placing prepared sperm directly into the uterus around ovulation. IUI works best if you have mild fertility challenges, regular ovulation, open fallopian tubes, and reasonably healthy sperm parameters. Read our step-by-step guide on the IUI procedure here.
IVF is a much more controlled and proactive approach. In an IVF cycle, eggs are retrieved from the ovaries and fertilized with sperm in a laboratory setting. This allows embryologists to monitor the fertilization process and select the healthiest embryos to transfer back into the uterus. IVF has higher success rates because fertilisation, embryo development, and timing are carefully monitored.
How Many IUI Cycles Are Usually Recommended
Most fertility specialists recommend three to four IUI cycles. If pregnancy does not occur within these attempts, the chances of success with further IUIs reduce significantly. Instead of repeating cycles without change, this is the stage where outcomes should be reviewed. Factors such as egg response, sperm quality, and uterine conditions need reassessment before deciding the next step.
Signs It May Be Time to Move from IUI to IVF
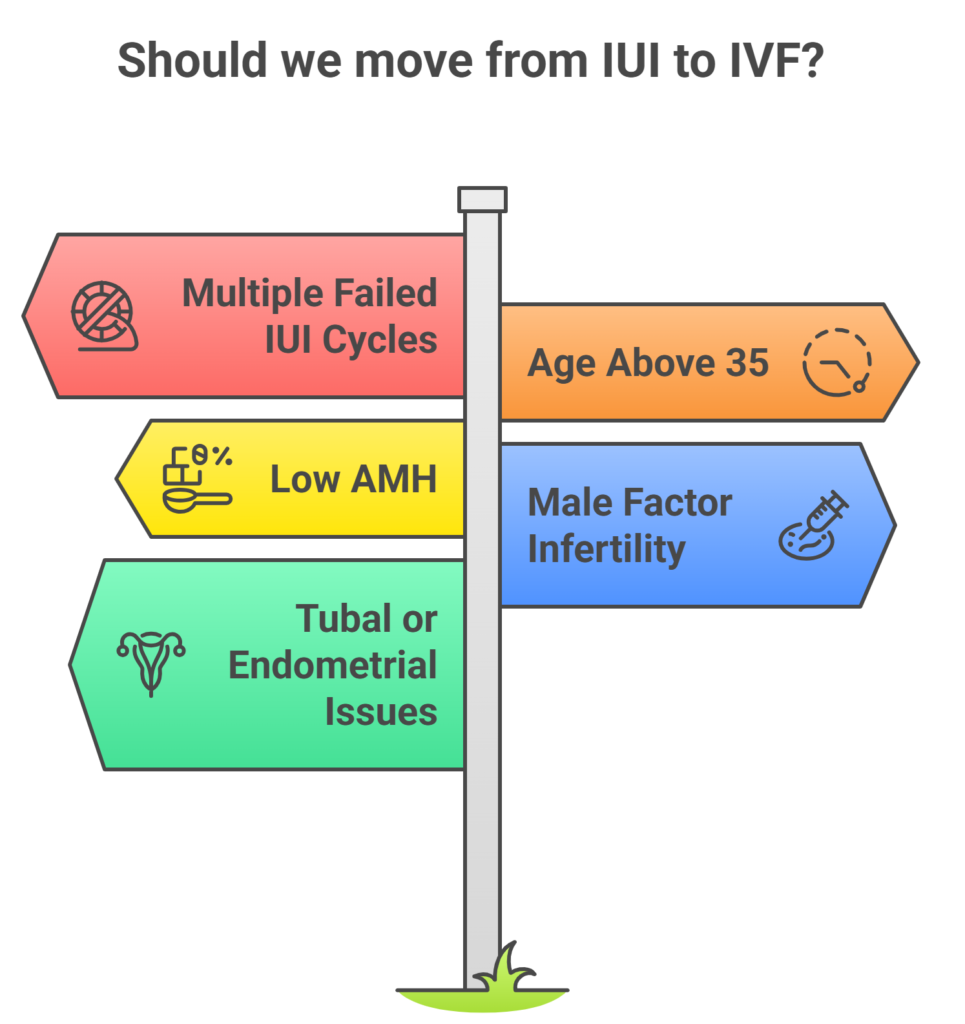 Every couple’s fertility journey is unique, but there are several clear indicators that IVF might be a more effective option for you.
Every couple’s fertility journey is unique, but there are several clear indicators that IVF might be a more effective option for you.
Multiple Failed IUI Cycles
If you have completed three or more properly timed IUI cycles without success, undergoing more IUI cycles will usually add emotional strain without improving results. You can have underlying issues related to egg/sperm quality or even how the embryo interacts with the uterine lining.
Age Above 35
Age directly affects egg quality. After 35, fertility declines faster, making time an important factor. Because IVF has a higher success rate per attempt, many specialists recommend moving to IVF sooner to maximize the chances of success while egg quality is still optimal.
Low AMH or Reduced Ovarian Reserve
If blood tests show a low Anti-Mullerian Hormone (AMH) level, it indicates a lower egg count. In these cases, IVF is often preferred because it allows doctors to retrieve as many eggs as possible in a single cycle and potentially freeze extra embryos for the future.
Male Factor Infertility
IUI requires a certain threshold of healthy, motile sperm to be effective. If sperm counts are low or if there are significant issues with morphology, the sperm may still struggle to reach and penetrate the egg naturally. IVF, specifically with ICSI (Intracytoplasmic Sperm Injection), can solve this by injecting a single healthy sperm directly into the egg.
Tubal or Endometrial Issues
When the fallopian tubes are damaged, or when moderate to severe endometriosis is present, the natural pathway that IUI depends on does not always function as it should. In these situations, continuing with IUI may only lead to more waiting without real progress. IVF can be a more effective next step because it bypasses the fallopian tubes completely and allows treatment to move forward in a more controlled way.
Emotional and Financial Considerations
When you are faced with multiple failed IUI cycles, it can lead to emotional fatigue. The uncertainty of waiting every month to know whether you are pregnant or not can be more draining than the treatment itself.
Financially, while IUI is cheaper per cycle, the costs can add up quickly. In some situations, moving to IVF earlier can be more cost effective and emotionally sustainable in the long run. Read our blog to learn more about IVF costs in Vizag.
Why Timing Matters More Than Trying One More IUI
It is common to want to try “just one more IUI” because it feels easier. If you spend a year or two on IUI without success, your age or ovarian reserve may change in that time, potentially making IVF less effective than it would have been if you started sooner. Fertility treatment tends to work best when there is a clear plan in place, rather than repeating the same steps without stopping to reassess what is actually working. Studies have shown that IVF often results in about twice as many clinical pregnancies per cycle compared to IUI. Moving to IVF at the right time can improve outcomes and also reduce the emotional strain that comes with months of uncertainty.
Do not view moving from IUI to IVF as a failure. It is a positive step forward when guided by the right medical advice. By making an informed and timely decision, you are taking charge of your journey and putting yourself in the best possible position to grow your family.
Couples across Visakhapatnam, Kakinada, Rajahmundry, Vizianagaram, and Anakapalli can seek personalised guidance at London IVF Centre, where experienced specialists focus on timely decisions, transparent counselling, and compassionate fertility care.
January 13, 2026
Have you decided to try IVF? If yes, then you might have several questions about the procedure, one of them would be “Will it hurt?” It is quite normal to worry about any pain or discomfort you might face. You might have anxiety around the treatment, as you may not know what happens exactly during each step. When you understand the entire IVF process step by step, your fear will reduce, and you will realise that the experience is quite manageable.
Does IVF Hurt?
Honestly, IVF is not something that is severely painful. There are a series of steps involved in IVF treatment, and some women might face mild, brief discomfort at certain stages, while others might not feel anything. Your experience with IVF will depend on your own pain threshold, how your body responds to hormones, and even your emotional state.
Modern fertility centers deeply care about patient discomfort and keep the process smooth and gentle as far as possible. Doctors monitor you closely, adjust medicines if needed, and make sure you never feel overwhelmed.
Understanding Pain Levels at Each Stage of IVF
IVF has several different stages, and when you know what to expect at each stage, the experience becomes much less intimidating. Here is how each part of the process typically feels.
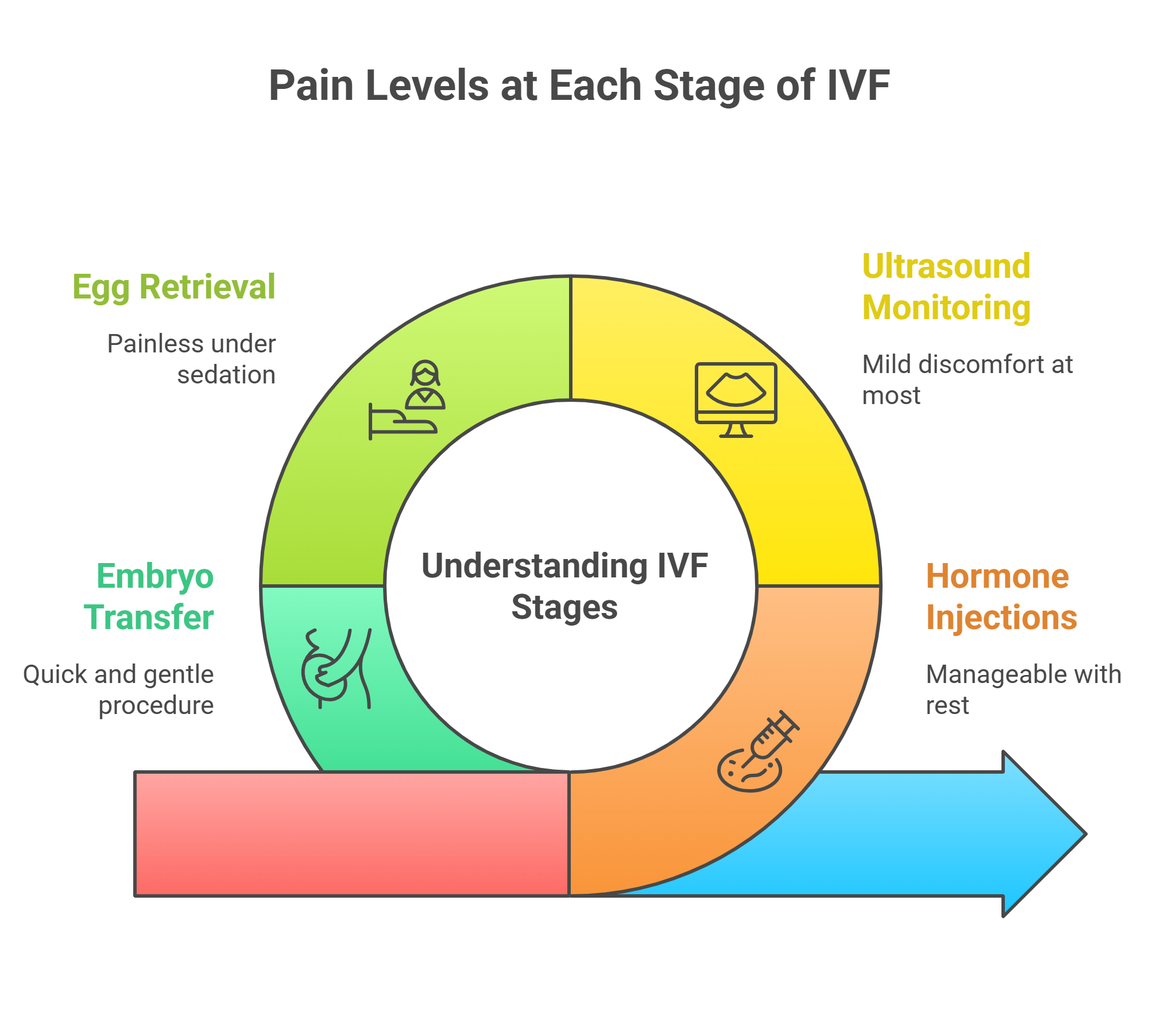 Hormone Injections
Hormone Injections
The thought of getting an injection can be quite scary for some people. But do not worry, the needles of these injections are thin and are given just under the skin, typically in your tummy or thigh. You might feel a quick pinch, similar to a finger-prick test. Your skin may feel slightly tender, and some women experience bloating, a sense of heaviness, or mood swings due to the hormones. These symptoms vary from person to person, but the majority of women find this stage manageable with rest and self-care.
Ultrasound Monitoring
Ultrasound scans are an important part of IVF because they help doctors track how your follicles are growing. These scans are not painful. At most, you may feel a little pressure or mild discomfort during an internal scan, especially if your bladder is full.
Egg Retrieval
Egg retrieval is the step where you might expect the most discomfort. The procedure is performed under light sedation or anaesthesia, which means that you will be comfortably asleep and feel nothing. After you wake up, you might experience period-like cramps, bloating, or light spotting for a day or two. Take rest for a day or two and use a heating pad or pain relief medicine prescribed by the doctor for cramps.
Embryo Transfer
Embryo transfer in IVF is a quick, simple, and gentle procedure. The procedure feels similar to a routine gynaecological exam. There is no need for anesthesia, and the whole process takes about 5-10 minutes. The only time you may feel slight discomfort is if you are asked to keep your bladder full, which helps the doctor get a clearer view during the procedure.
Is IVF More Painful for Women with Certain Conditions?
Now, another question you might have is if I have certain conditions like PCOS, endometriosis, low ovarian reserve, or a history of painful periods, then will IVF be more painful? While these conditions can sometimes make monitoring or retrieval slightly more sensitive, it doesn’t mean the process becomes painful. As these conditions impact how your body responds to hormones, you might feel a little more bloating or cramping than others.
Your doctor will be aware of your medical history and can adjust treatment plans to ensure that your body responds safely.
How IVF Clinics Help Manage Pain and Discomfort
The best fertility clinic will help you manage both physical and emotional discomfort. Here is what you can expect from the top IVF clinics in Vizag:
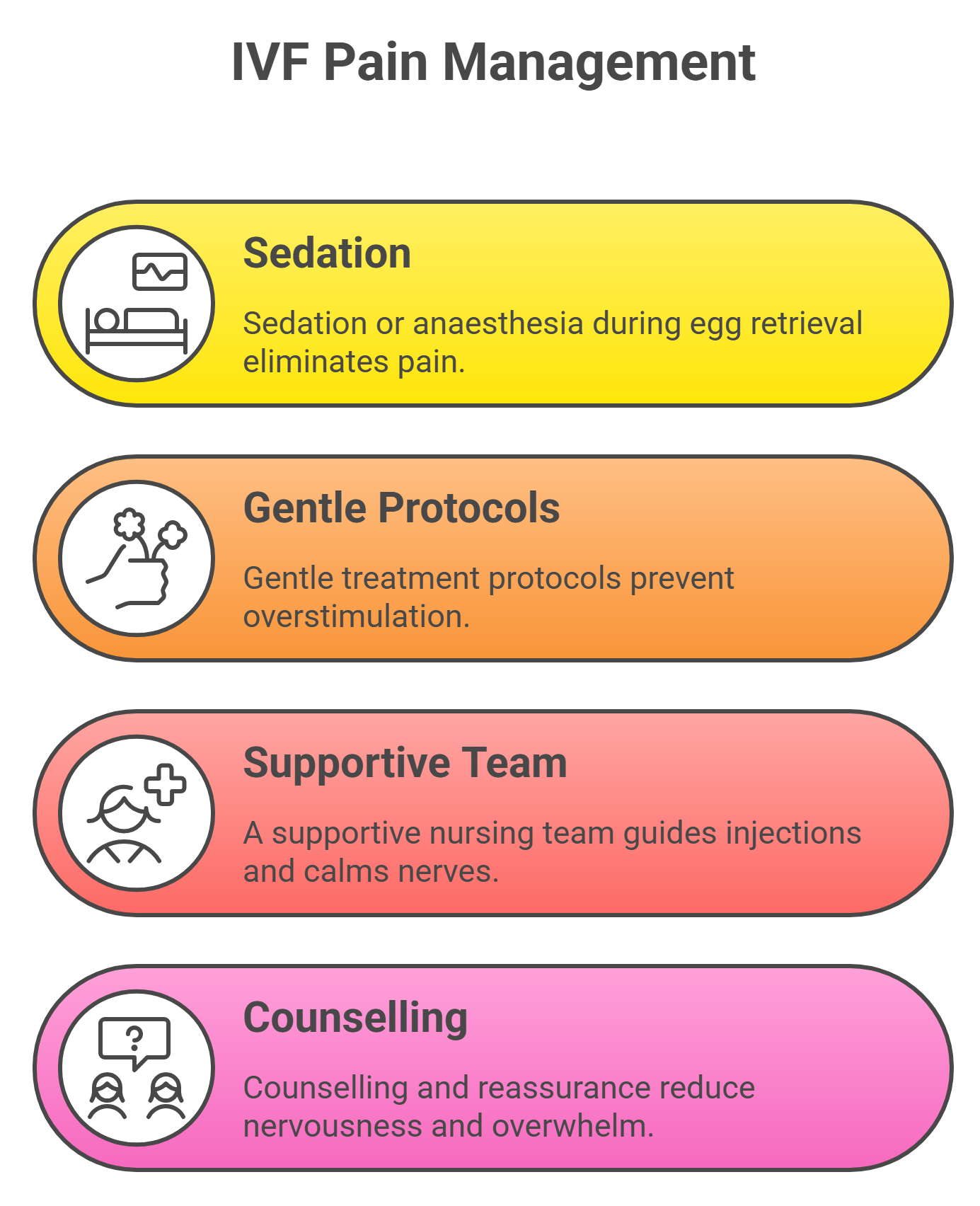
- Sedation or anaesthesia during egg retrieval, so you feel no pain.
- Gentle treatment protocols to avoid overstimulation.
- A supportive nursing team that guides you through injections and helps you stay calm.
- Counselling and reassurance that make a significant difference when you are nervous or overwhelmed.
Recent research also supports the effectiveness of these modern approaches. A 2025 randomized study by US Fertility found that patients who received an improved pain-management protocol after egg retrieval reported significantly lower pain levels and needed far fewer narcotics, without affecting embryo-transfer success.
When Should You Contact Your Doctor?
Many symptoms during IVF are completely normal. You may notice mild cramps, slight spotting, bloating, changes in mood, or some sensitivity where the injections were given. These effects are usually short-lived and simply indicate your body’s response to the hormonal treatment.
However, there are certain symptoms that require medical attention. You should contact your doctor if you experience severe or increasing pain, heavy bleeding, fever or chills, difficulty breathing, or extreme bloating that gets worse instead of settling. These signs are uncommon, but it is always safer to reach out early rather than wait.
With the right guidance, a supportive medical team, and clear communication, the entire process becomes easy to navigate. The best IVF clinics will prioritise safety, comfort, and personalised care.
Are you ready to start your IVF journey? At London IVF Centre, our team ensures that every step of your treatment is gentle, personalised, and supportive. Book a consultation today.
December 14, 2025
So, you have just finished your embryo transfer and are now entering an important but gentle part of your IVF journey. First off, take a deep breath. It’s completely normal for your mind to now race towards the next step, fixating on every little twinge and wondering, “Am I doing this right?” The first 48 hours can feel like a lifetime, wrapped in a mix of hope and anxiety.
Let’s get one thing straight from the start: while these hours feel crucial, your ultimate success doesn’t hinge on lying perfectly still for two days. This guide offers you simple, practical steps to navigate this waiting period with confidence and care.
What’s Actually Happening Inside Your Body after IVF?
After the embryo transfer, your little embryo is embarking on its own big adventure. It’s floating in the uterine cavity, looking for the perfect, cosy spot to implant. This process, called implantation, doesn’t happen instantly. It’s a delicate dance between your embryo and your uterine lining, one that takes several days to complete.
Many of us grew up hearing the myth of strict bed rest. But modern research tells a different story. Research shows that you don’t need complete bed rest, gentle movement actually supports healthy blood flow to your uterus, which is a good thing. You might feel some mild cramping, a bit of fatigue, or even light spotting. Your body is doing its job. Trust it.
Resting Smart: Your Body’s Best Friend
We said “no” to strict bed rest, but we give a resounding “yes” to smart rest. Your body has been through a lot. Plan for light rest. Think of it as a lazy weekend. You might spend a few hours on the sofa with a good book or your favourite feel-good series. But you can also get up to make a cup of tea, walk gently to the bathroom, or putter around the kitchen. This light activity prevents stiffness, supports circulation, and can actually ease anxiety better than staying completely stationary.
So, what does “light activity” really mean after IVF implantation?
Feel free to:
- Take slow, gentle walks around your home.
- Do some light stretching.
- Move through your day at a relaxed pace.
For now, press pause on:
- High-intensity workouts, running, or cycling.
- Lifting anything heavier than a full kettle.
- Any activity that jars your body or strains your core.
Nourishing Your Body and Soul
You don’t need a special “implantation diet,” but choosing comforting, nutritious foods can make a world of difference.
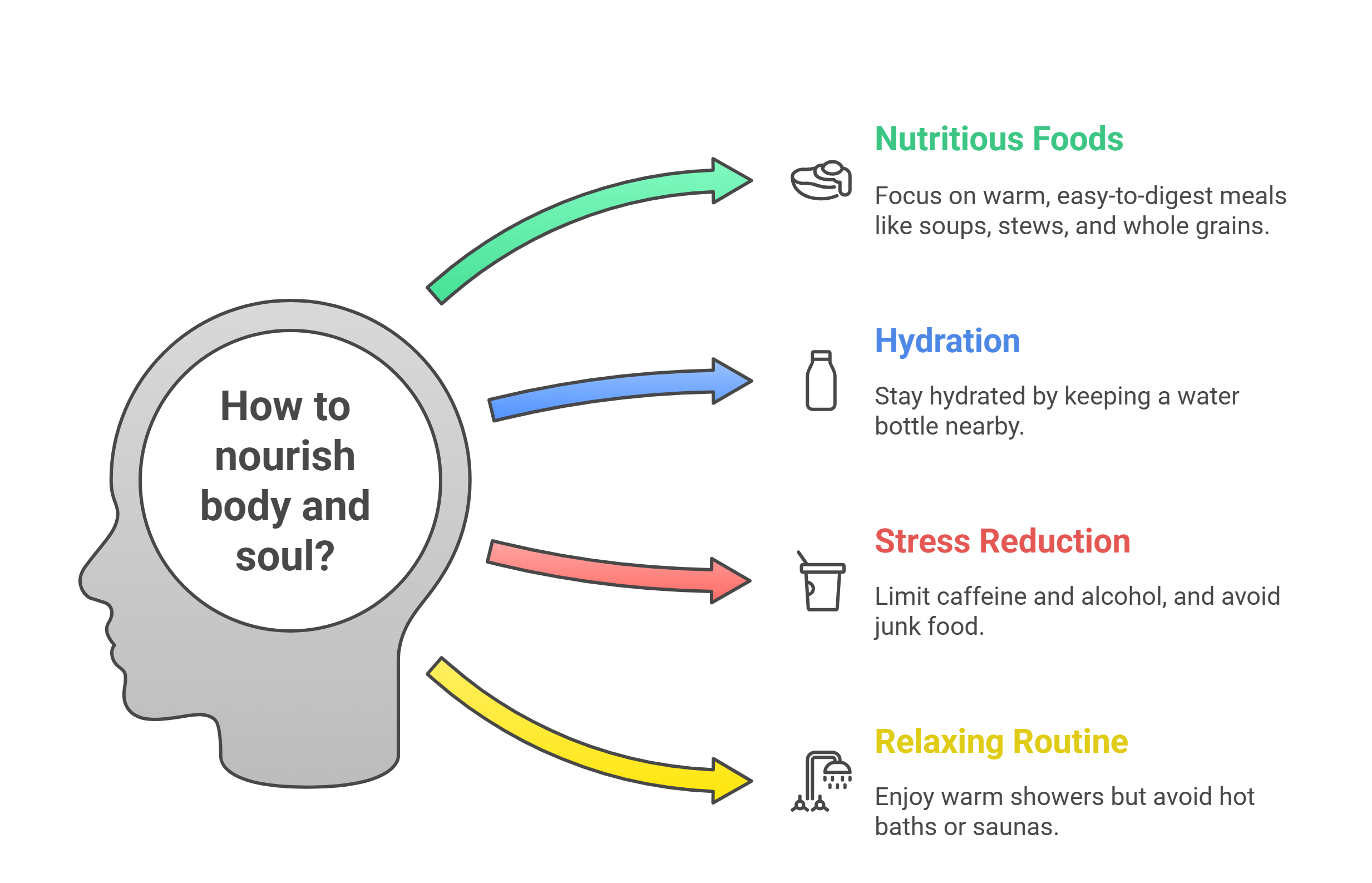
Focus on warm, easy-to-digest meals. Soups, stews, whole grains like oats or quinoa, and steamed fruits feel nurturing. Stay hydrated, keep a water bottle by your side. Good hydration helps with everything from blood flow to keeping those pesky progesterone-related bloating symptoms at bay. Read more about nutrition during IVF pregnancy here.
It’s also a good time to limit things that can add stress to your system. Cut back on caffeine, avoid alcohol completely, and maybe swap the junk food for something that makes your body feel truly nourished. And for your daily routine? A warm shower is perfectly fine and wonderfully relaxing, but skip the hot bath or sauna for now.
Your Emotional Well-Being Matters Just As Much
We talk so much about physical rest, but your mind needs a break, too. The emotional weight of this waiting period is real.
Find small, practical ways to gift your mind some calm. Try a simple breathing exercise: inhale for four counts, hold for four, and exhale for six. Lose yourself in a light novel or a calming playlist. Watch a comedy that makes you laugh out loud. The goal isn’t to police your every thought, but to gently guide your focus away from the “what ifs” and towards a positive mental space.
Partner Support During IVF: You are In This Together
If you have a partner, this is their time to shine. Their role isn’t to fix the outcome, no one can do that, but to be your anchor. They can handle the chores, make meals, and be a calm presence.
Open communication is everything. Talk about how you are feeling, both the hope and the fear. Sharing this burden makes it lighter for both of you and strengthens your connection during this intense time.
The Non-Negotiables: Medication & Follow-Up
This is the most important part: take your medications as prescribed. Progesterone supplements are the cornerstone of supporting your uterine lining. Set an alarm on your phone, use a pill organiser, create a little ritual around it, do whatever it takes to stay on schedule.
Finally, know when to call your clinic. Mild cramping is normal. But if you experience severe pain, heavy bleeding (soaking a pad), or a fever, don’t hesitate to reach out for professional guidance.
You have got this. Be kind to yourself, trust the process, and take it one gentle step at a time.
If you want personalised guidance throughout your IVF journey, the team at London IVF Centre is here to help with expert care and compassionate support. Reach out whenever you need us.
November 27, 2025
If you have just started your fertility journey, one of the most common treatments that might be recommended is Intrauterine Insemination (IUI). It is a simple procedure where specially prepared sperm are directly placed inside the uterus around the time of ovulation. This helps increase the chances of the sperm meeting the egg, especially when timing or sperm count is a concern.
IUI is less invasive than IVF and more affordable; it boosts the chances of conception when natural methods are not working. If you have decided to go with IUI, chances are that you are focusing only on the medical side. But what you may not realize is that lifestyle choices play a major role in how well the treatment works. Even small, consistent changes in diet, exercise, and daily habits can support IUI and improve your chances of conceiving.
Nutrition and Diet for IUI
Good nutrition is very important for your reproductive system to function well. Your diet directly impacts hormone balance, egg quality, and sperm health. Including certain foods in your diet like whole grains, lean proteins, healthy fats, and low-glycemic foods, supports the body during fertility treatments.
There are certain nutrients that are important during the IUI journey, like:
- Folic acid supports cell development and reduces the risk of birth defects.
- Vitamin D improves reproductive hormone levels in both men and women.
- Antioxidants such as vitamin C and E protect eggs and sperm from oxidative stress.
You can include foods like brown rice, quinoa, lentils, beans, eggs, and fresh fruits and vegetables in your diet. Apart from this, omega-3 fatty acids from fish, flaxseeds, and walnuts help reduce inflammation and promote healthy hormone production. Read our blog, 14 Best Fertility Boosting Foods for Couples in Andhra Pradesh, to learn more about fertility-enhancing foods.
In addition to a balanced diet, you need to ensure that you are properly hydrated. Aim for at least eight glasses of water a day to support healthy cervical mucus and overall body function. Limit caffeine and alcohol intake, as they can interfere with hormone levels.
Exercise and Physical Activity
Regular physical activity relieves stress and helps manage weight. This is important as a healthy BMI supports better hormonal balance and ovulation. Activities like walking, yoga, swimming, and light strength training can boost blood flow and support reproductive health.
However, balance is essential. Over-exercising or high-intensity workouts can disrupt menstrual cycles and reduce sperm count. The goal is not to push your limits but to keep your body strong, flexible, and relaxed. A 30-minute walk or a gentle yoga session a few times a week can be more beneficial than intense gym routines. You can read more about the effect of exercise on fertility here.
Stress and Emotional Well-being
Fertility treatments can be quite stressful, and high stress levels can interfere with ovulation, affect sperm health, and make it difficult for you to stay positive. To improve the chances of IUI success, you have to find ways to manage stress. Some of the stress-relieving techniques you can explore are:
- Meditation: commit to 10-15 minutes a day of meditation or deep breathing exercises.
- Journaling: write down your thoughts, feelings, and worries to process emotions.
- Seek Support: talk to a neutral party, like a counselor or therapist, or join a support group. Sharing your feelings with others who understand the journey can reduce emotional pressure.
Remember, emotional health and physical health are closely connected, and both matter during IUI.
Avoid Harmful Substances
If you are preparing for or undergoing IUI, it is crucial to stay away from substances that can affect fertility.
- Quit Smoking and Limit Alcohol: Both smoking (active and passive) and alcohol consumption significantly decrease fertility in both men and women, and must be avoided.
- Be Cautious with Medicines: Always consult your fertility specialist about any over-the-counter medicines, herbal supplements, or vitamins you plan to take. Some common medications can interfere with fertility drugs or implantation.
- Reduce Exposure to Toxins: You can reduce your exposure by choosing BPA-free plastics and using natural cleaning products where possible.
Shared Responsibility: The Male Partner’s Role
The outcome of fertility treatments depends on the lifestyle choices of both partners. Sperm health improves with a balanced diet, regular exercise, and proper hydration. Men should include antioxidant-rich foods like berries, nuts, and leafy greens to protect sperm from oxidative stress.
Avoiding prolonged heat exposure is also important. Hot tubs, saunas, or even keeping a laptop on the lap for long hours can affect sperm production. Getting enough sleep, managing stress, and maintaining a healthy weight all contribute to better sperm quality.
IUI is a good first step in your fertility journey; however, its success depends more than just on the medical procedure. Nutrition, exercise, stress management, and healthy daily habits all work together to give you a chance of a successful pregnancy.
If you are considering IUI, the expert team at London IVF Centre can guide you through every step with personalised care and holistic support. Reach out today to take your first step toward parenthood.
November 6, 2025
If you are a couple in your late 30s or early 40s and have been trying to get pregnant without any luck, then the conversation around infertility must have come up. Generally, many people think that infertility is a woman’s problem, but male infertility is a reason for nearly half of the infertility cases.
The reason for male infertility is not always medical, as your lifestyle choices also play a role in it. One of the lifestyle factors that plays an important role in sperm health and hormonal balance is exercise. Though exercise is important, both too little and too much exercise can impact your fertility.
Exercising the right way can help boost circulation, support testosterone levels, and help maintain a healthy weight. Let’s look at how exercise affects male fertility and how you can find a healthy balance that supports both fitness and reproductive health.
What Causes Male Infertility
There are several factors that can lead to infertility in males. Some of these are low sperm count, poor sperm motility, or abnormal sperm shape. Apart from these, hormonal imbalances, stress, and obesity can make things worse. Some medical conditions, such as varicocele, which is enlarged veins in the scrotum, or infections, also contribute to male infertility.
Your lifestyle choices also have a direct impact on fertility. If your diet is poor in nutrition, you are doing little or no physical activity, and are smoking and drinking alcohol excessively, then it can harm the sperm quality.
The Positive Role of Exercise on Male Fertility
Exercise, when done in moderation, can have a positive impact on reproductive health. Regular exercise boosts blood flow, supports heart health, and helps maintain optimal testosterone levels. When you remain active, you are able to maintain a healthy weight, reducing the risk of hormonal imbalance. Regular exercise also reduces oxidative stress that can damage sperm DNA. Lower oxidative stress means healthier sperm DNA and a better chance of conception.
Some of the best activities for improving fertility include brisk walking, swimming, yoga, cycling in moderation, and light resistance training. These exercises promote hormonal balance without putting excessive strain on the body. You should focus on keeping your body active without getting exhausted.
When Exercise Can Harm Fertility
While moderate exercise is good for reproductive health, overdoing it can have the opposite effect. Overtraining can lead to low testosterone and reduced sperm production. If you spend hours daily doing high-intensity workouts, you may experience fatigue, hormonal disruption, and even reduced libido.
Prolonged exercise can also increase heat and stress in the testicular area, leading to fertility challenges. Another important aspect to consider is the use of anabolic steroids or performance-enhancing substances. These may boost muscle mass in the short term, but can severely reduce or even stop sperm production. Recovery is possible once the use stops, but it may take several months or longer.
Balancing Fitness and Fertility
Your goal should be to find a healthy balance between physical fitness and fertility. You can plan to do a 30 to 45-minute workout 4 to 5 times a week. You need to keep your body active without overstraining it. Giving your body the time to rest and recover is equally important. Intense exercise without enough downtime does not allow the body to repair itself, leading to hormonal imbalances.
A balanced diet is equally important. Foods rich in antioxidants, vitamins, and minerals support sperm health. Eat plenty of fruits, vegetables, whole grains, nuts, and lean protein. Also, try to include omega-3 fatty acids from fish or flaxseeds in your diet to improve sperm function.
You also need to focus on getting quality sleep and keeping your body hydrated so that your body is able to function smoothly. Exercise is not a magical solution for infertility but a part of a comprehensive fertility approach.
Lifestyle Habits That Complement Exercise
Exercise is not a magical solution for infertility, but a part of a comprehensive fertility approach that includes lifestyle changes. Some of the lifestyle habits that can improve your chances of getting pregnant include:
1. Quitting smoking, limiting alcohol, and avoiding heat exposure to improve sperm health.
2. Keeping stress levels in check through relaxation techniques. Meditation, yoga, or spending time in nature can calm the nervous system and support fertility.
At London IVF Centre our fertility specialists can guide you on how to align your lifestyle choices with treatment goals.
When to Seek Help
Even after several months of making lifestyle changes and following a healthy routine is not helping, then it may be time to consult a fertility specialist. Doing so will save valuable time and provide clarity. A fertility specialist will provide you with comprehensive male fertility assessments, including semen analysis, hormonal evaluation, and personalized treatment plans.
Exercise has a powerful influence on male fertility, but the key lies in moderation. Staying active improves hormone balance, reduces stress, and supports sperm health. Overdoing it, however, can have the opposite effect.
If you continue to face challenges, book an appointment at London IVF Centre to identify the root cause and get personalized solutions.
November 3, 2025
If you are trying to conceive for a long time but are not successful, you need to check for factors related to male infertility as well. One of the most common factors for male infertility is low sperm count. Even though it can sound worrying, low sperm count is quite common and often treatable. What you need to focus on is to look for low sperm count signs and get the right medical help without any delay.
What Does a Low Sperm Count Mean?
In simple words, a low sperm count means that a man’s semen has fewer sperm than what is considered as normal. A healthy count is about 15 million sperm per milliliter or higher. Anything lower can make it harder to conceive naturally.
However, it’s not just the number of sperms that matter when you are trying to get pregnant, the movement and shape of the sperm are also important. Even if you have a low sperm count, but they are healthy and active, pregnancy can still happen. That is why doctors usually start with a semen analysis. It is a straightforward test that gives a clear picture of sperm count, quality, and movement.
Common Low Sperm Count Signs
Even if you have a low sperm count, you might feel completely fine till you notice that you are having trouble conceiving. Still, your body often gives signals that something might be wrong.
Here are some signs of low sperm count to watch out for:
- Lower interest in sex than usual
- Trouble getting or maintaining an erection
- Pain, swelling, or a feeling of heaviness in the testicles
- Less facial or body hair than before
- Feeling unusually tired or low in energy
None of these symptoms confirm a low sperm count on their own, but they are reasons enough to get checked. If you and your partner have been trying to conceive for over a year (or six months if she is over 35), it is best to see a fertility specialist as early as you can.
Why Does It Happen?
Low sperm count can have many different causes, and sometimes it’s a mix of several factors.
There can be some medical reasons like varicocele (enlarged veins in the scrotum), hormonal imbalances, or infections that affect sperm production. Some men are born with genetic factors that influence fertility, while others experience issues like ejaculatory blockages.
Lifestyle habits also play a big role. Smoking, alcohol, poor diet, stress, and lack of exercise can all lower sperm quality. Long work hours, irregular sleep, or constantly being exposed to stress can gradually affect hormone levels.
Environmental exposure matters too. Sitting for long hours with a laptop on the lap, working in high-temperature environments, or coming into contact with chemicals and toxins can reduce sperm count.
Apart from the above, certain medications or health conditions like diabetes and thyroid disorders can also interfere with sperm production.
Getting the Right Diagnosis
If any of the low sperm count signs sound familiar, the next step is to get tested. A semen analysis gives the most accurate starting point. The test measures sperm count, movement, and shape.
Depending on the findings, your doctor might suggest additional tests such as hormone testing, a scrotal ultrasound, or even genetic screening. These help find the exact cause so that treatment can be tailored to you. It is best to consult a fertility specialist or an andrologist, as they focus specifically on male reproductive health.
Treatment for Low Sperm Count
Simple lifestyle changes can go a long way. Eating a balanced diet with plenty of antioxidants, staying active, maintaining a healthy weight, quitting smoking and alcohol, and finding healthy ways to manage stress can all help boost sperm health. Even getting enough sleep makes a difference.
When medical treatment is needed, doctors may suggest hormonal therapy, antibiotics (if an infection is present), or surgery for conditions like varicocele. In other cases, specific medications can help regulate hormones or improve sperm production.
If natural conception still seems difficult, fertility treatments offer excellent success rates. Techniques like IUI (Intrauterine Insemination), IVF (In Vitro Fertilization), and ICSI (Intracytoplasmic Sperm Injection) have helped thousands of couples conceive, even when sperm counts are very low.
Low sperm count is not something to be ashamed of. It is a medical condition, and like most health issues, it can be treated with the right care. Recognizing low sperm count signs early and speaking to a specialist can help you get pregnant.
If you have been trying to conceive and suspect low sperm count could be a reason, then book a consultation and explore advanced fertility treatments, personalized plans, and supportive care.
October 16, 2025
If you are facing fertility challenges, don’t be disheartened; you are not alone. Around 60–80 million couples suffer from infertility globally, out of which 15–20 million are in India. Like many other couples, you might be considering different fertility treatment options like IVF, ICSI, IUI, etc. You can even check out our blog here to find the best option for you.
In Vitro Fertilization (IVF) gives hope to countless couples looking to start a family. Though IVF can help you in your journey to becoming a parent, it is not as easy and straightforward. You might have to face failed IVF cycles or lose a pregnancy. Going through something like this can be very painful and challenging.
But don’t worry, there are some techniques like Preimplantation Genetic Testing for Aneuploidies (PGT-A) and Preimplantation Genetic Diagnosis (PGD) that help refine the embryo selection process and improve your chances of a healthy pregnancy.
What Is Genetic Testing in IVF?
Before we go any further, let us first understand what genetic testing is. During IVF, doctors may recommend genetic testing. They examine the embryos for abnormalities and select only those with 46 chromosomes and no inherited genetic conditions for transfer. This increases the chances of implantation as well as the chances of the embryo growing into a healthy baby.
There are two main types of genetic testing: Preimplantation Genetic Testing for Aneuploidy (PGT-A) and Preimplantation Genetic Diagnosis (PGD). PGT-A focuses on checking for the right number of chromosomes, while PGD looks for specific inherited disorders.
Types of Genetic Testing Used in IVF
Depending upon your situation, your doctor will recommend either PGT-A or PGD. Let us have a look at how they differ from each other.
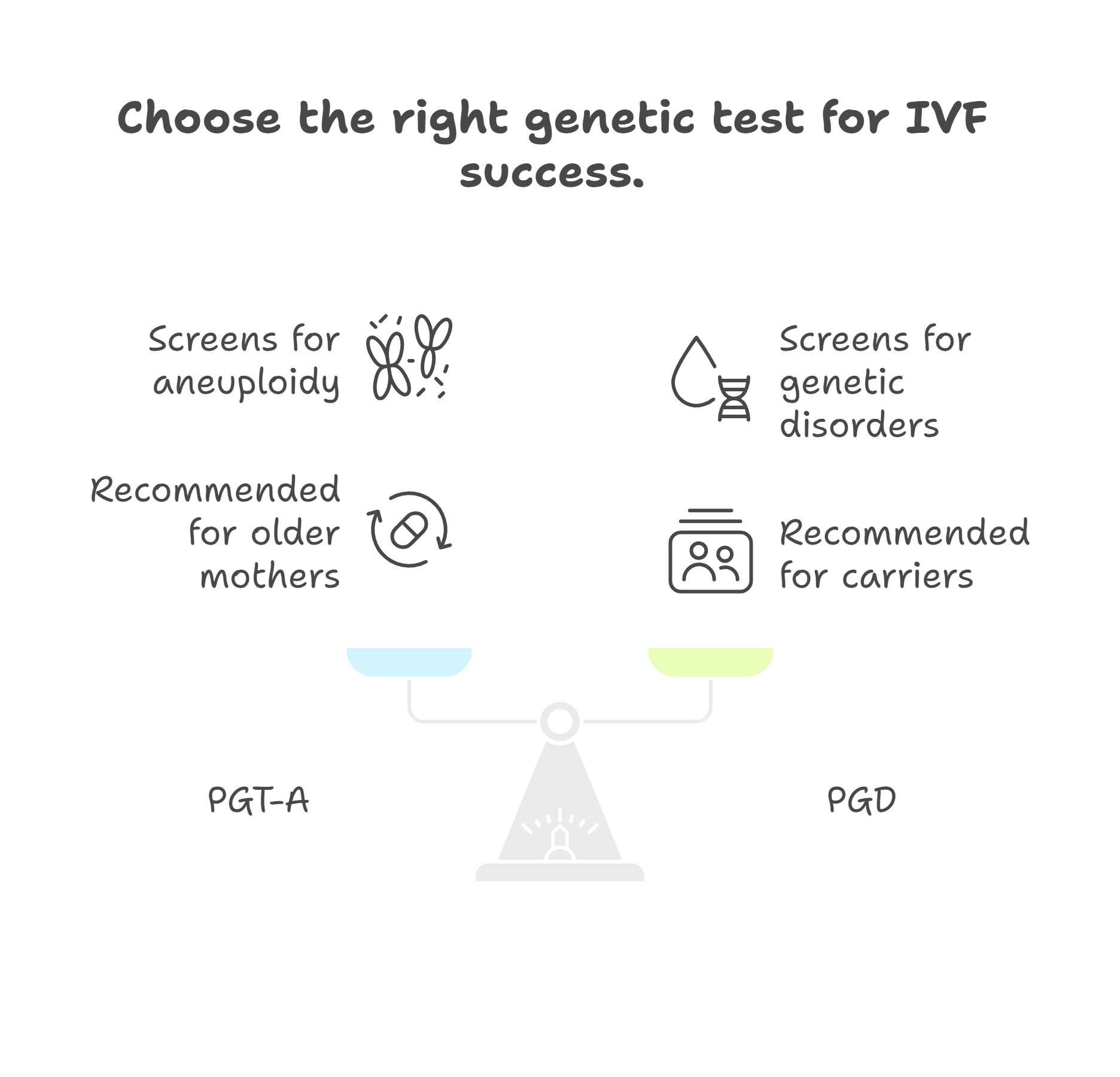
Preimplantation Genetic Testing for Aneuploidies (PGT-A)
In PGT-A, the embryos will be screened for aneuploidy, which means missing or extra chromosomes. This test is especially helpful if you are over 35, as the risk of chromosomal errors increases with age. It is also often recommended for couples who have faced failed IVF cycles.
Preimplantation Genetic Diagnosis (PGD)
PGD screens the embryo for specific inherited genetic disorders. Doctors usually recommend it if you or your partner carries a known genetic condition such as thalassemia, sickle cell anemia, or cystic fibrosis. PGD can check embryos for those exact mutations, ensuring that only the embryos without the disease are transferred. It reduces the risk of passing on inherited disorders to the next generation.
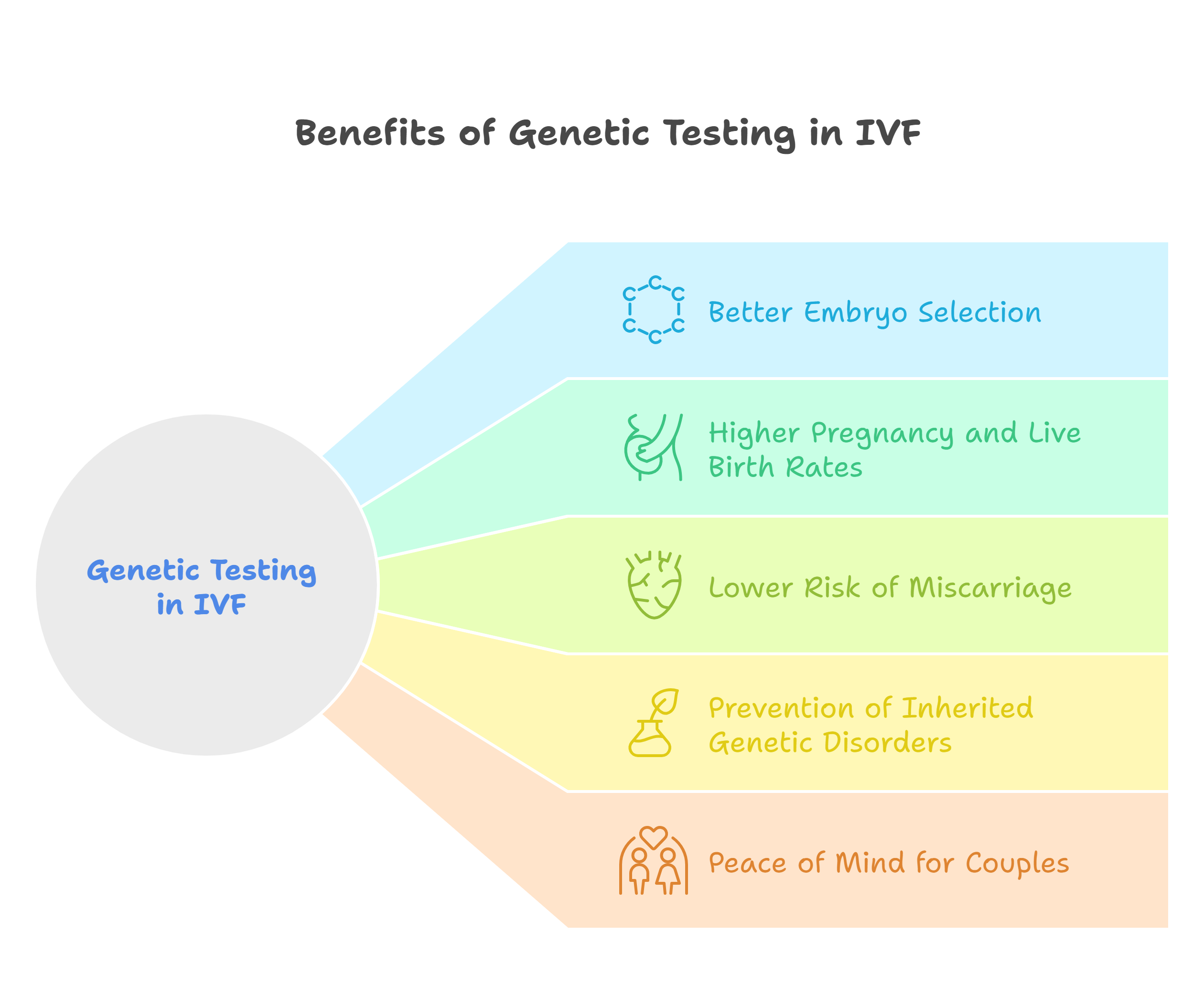
Why PGT-A and PGD matter in IVF?
Chromosomal abnormalities in embryos are one of the main reasons why some IVF cycles fail or lead to miscarriages. In fact, studies suggest that approximately 50% of miscarriages are due to chromosomal abnormalities. As the age of the couples increases, the risk of aneuploidy, i.e., having a lower or higher number of chromosomes than normal, increases.
Doctors can use PGT-A and PGD to identify which embryos are genetically healthy and most likely to implant successfully. Apart from improving plantation rates, PGT-A reduces the risk of miscarriages. Genetic testing can have emotional benefits for couples as well. Going through this process makes you feel more confident as you know that the embryos being transferred have been carefully screened.
Who Should Consider PGT-A/PGD?
Genetic testing is not always necessary for every IVF case, but there are certain situations where it can make a significant difference. Doctors often recommend PGT-A or PGD when they identify risks that could affect embryo health. Some common scenarios include:
- Couples with multiple failed IVF attempts If earlier cycles did not work despite transferring good-quality embryos, genetic testing can help uncover whether chromosomal issues were the hidden cause.
- Women over the age of 35 As women get older, the chances of chromosomal abnormalities in eggs increase. PGT-A helps ensure that only the healthiest embryos are chosen for transfer.
- Couples with a family history of genetic diseases
- Families affected by conditions such as thalassemia or cystic fibrosis can use PGD to ensure they do not pass these disorders on to their child.
- Patients with recurrent miscarriages Losing a pregnancy more than once can be devastating. In many cases, miscarriages are linked to chromosomal problems. PGT-A can reduce this risk by identifying healthy embryos.
- Male infertility cases Sometimes, sperm abnormalities can increase the likelihood of genetic errors in embryos. Testing helps detect these issues early.
For many couples, IVF is a journey filled with hope, patience, and resilience. Adding genetic testing through PGT-A or PGD can make this journey smoother by increasing the chances of success and reducing the risks that often bring heartbreak. These advanced techniques help doctors identify the healthiest embryos, prevent certain genetic conditions, and give couples a stronger sense of confidence moving forward.
While PGT-A and PGD cannot promise a 100 percent outcome, they have proven to be valuable tools in improving IVF success rates.
At London IVF, we are committed to supporting every couple with the latest technology, compassionate care, and personalized guidance. If you are considering IVF or want to explore whether PGT-A or PGD could help in your journey, book a consultation today.
September 2, 2025